What Excess Sugar Does to Your Metabolism, Brain, and Skin (Beyond Weight Gain)

Most people think sugar is a weight problem.
It’s not.
Excess sugar changes how your metabolism functions, how your brain regulates energy and mood, and how your skin ages at a structural level. And it does this long before visible weight gain becomes the issue.
The effects are biochemical, not cosmetic. They influence insulin signaling, inflammatory pathways, cellular repair, and even how your body interprets stress.
This isn’t about fear or elimination diets. It’s about understanding what happens physiologically when sugar intake exceeds what your body can safely process.
Once you understand that, your food choices stop being about discipline — and start being about biology.
Let’s begin with metabolism.
Quick Summary
Excess sugar doesn’t just cause weight gain — it disrupts metabolic signaling long before the scale changes. Frequent blood sugar spikes increase insulin resistance, strain the liver (promoting fat accumulation), and reduce metabolic flexibility. In the brain, unstable glucose affects focus, mood, and dopamine sensitivity. In the skin, repeated glucose exposure accelerates glycation, stiffening collagen and contributing to premature aging.
The issue isn’t one dessert — it’s chronic elevation without recovery. Over time, excess sugar shifts your body from resilient regulation to reactive compensation.
Disclosure: The information provided is for educational purposes only and not intended as medical advice. Consult a healthcare professional before making any changes to your health routine.
- Quick Summary
- The Real Problem Isn’t Weight — It’s Signaling
- First Shift: Blood Sugar Instability
- Second Shift: The Liver Becomes Overloaded
- Third Shift: The Brain’s Energy System Changes
- Fourth Shift: Structural Aging Through Glycation
- When Sugar Becomes a Daily Regulator
- What “Excess” Actually Means
- Rebuilding Metabolic Resilience
- The Quiet Accumulation Effect
- Final Thoughts
- ❓ FAQs
The Real Problem Isn’t Weight — It’s Signaling
Most conversations about sugar start with calories. Or weight. Or self-control.
But excess sugar doesn’t begin by changing your body size. It begins by changing your signals.
Your body runs on messaging systems. Hormones tell cells when to store or release energy. Inflammatory molecules signal repair or defense. Neurotransmitters influence mood, focus, and motivation. None of these systems operate randomly. They respond to input.
Sugar is one of those inputs.
When sugar intake is occasional and paired with whole foods, the body adjusts. Blood glucose rises, insulin responds, and levels return to baseline. The system resets.
When intake is frequent — especially from added sugars and refined carbohydrates — those signals start firing more often than they were designed to.
Insulin rises more frequently. Stress hormones compensate for crashes. Inflammatory pathways activate. Reward circuits light up. And instead of brief adjustments, the body begins adapting to a new normal.
The issue isn’t a single spike.
It’s repetition.
Over time, the body recalibrates around those repeated signals. What was once a flexible system becomes reactive. What was once stable energy becomes cyclical. What was once occasional inflammation becomes background noise.
This is why the real concern with excess sugar isn’t cosmetic.
It’s regulatory.
And once regulation shifts, the first system to show strain is your blood sugar stability — which is where the cascade begins.
First Shift: Blood Sugar Instability

The first change excess sugar creates is not disease.
It’s instability.
Every time you consume added sugar, blood glucose rises. Your pancreas releases insulin to move that glucose into cells for immediate use or storage. In a healthy system, this rise and fall is controlled. Glucose increases, insulin responds, levels return to baseline.
The problem begins when this cycle happens repeatedly throughout the day.
Frequent spikes mean insulin is elevated more often. Over time, cells become less responsive to insulin. The body compensates by producing more — an early stage of insulin resistance that often requires intentional strategies for how to balance insulin naturally.
You may not see it on a lab test yet.
But you can feel it.
Energy becomes unpredictable.
You feel alert after eating — then foggy.
You crave something sweet mid-afternoon.
You wake up tired, even after sleeping.
When blood sugar drops quickly after a spike, the body releases stress hormones to stabilize it — reinforcing patterns seen in chronic nervous system dysregulation. Cortisol and adrenaline rise to bring glucose back into circulation. That “shaky,” anxious, irritable feeling after a crash isn’t psychological weakness. It’s biochemical compensation.
This pattern does three things over time:
- It increases fat storage, particularly around the abdomen.
- It narrows metabolic flexibility — the ability to burn fat between meals.
- It conditions the brain to associate sugar with stability.
At that point, sugar is no longer just a taste preference.
It becomes a regulator.
And when regulation depends on frequent glucose correction, the next system to feel the strain is the liver — which must process the overflow.
Second Shift: The Liver Becomes Overloaded
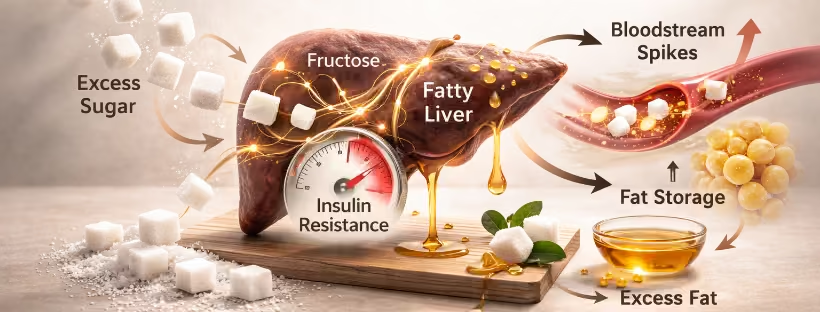
Once blood sugar becomes unstable, the liver absorbs much of the metabolic pressure.
Glucose can be used by nearly every cell in the body. Fructose — the other half of table sugar and a major component of high-fructose corn syrup — cannot. It is processed primarily in the liver.
In small amounts, this isn’t a problem. The liver converts fructose into usable energy intermediates. But when intake is high and frequent, the liver begins converting excess fructose into fat through a process called de novo lipogenesis.
This is not a dramatic event. It’s gradual.
Triglyceride levels begin to rise. Fat accumulates inside liver cells. Over time, this pattern is associated with increased liver fat accumulation — even in people who do not appear overweight.
What makes this shift significant is that the liver plays a central role in metabolic regulation. When it becomes overloaded:
- Blood lipid levels increase
- Insulin sensitivity declines further
- Inflammatory signaling rises
- Energy regulation becomes less efficient
The body becomes more dependent on frequent carbohydrate intake because fat oxidation — burning stored fat for energy — becomes less accessible.
This is known as metabolic inflexibility.
At this stage, sugar is no longer just causing spikes. It is altering how energy is stored and released.
And when energy regulation shifts, the brain begins adapting to that instability as well — which is where the next changes appear.
Third Shift: The Brain’s Energy System Changes

The brain depends on steady energy. It does not tolerate instability well.
When blood sugar rises and falls repeatedly, the brain adapts to that rhythm. At first, this feels like normal fatigue or irritability. Over time, it becomes a shift in how the brain regulates energy, mood, and reward.
One of the earliest changes involves insulin signaling in the brain.
Insulin doesn’t just move glucose into muscle and fat cells. In the brain, it plays a role in learning, memory formation, and neuronal repair. When peripheral insulin resistance develops, similar resistance can begin affecting brain tissue. The result is less efficient glucose uptake in certain regions, particularly those involved in memory and executive function.
This doesn’t present as sudden cognitive decline.
It shows up as:
- Brain fog
- Reduced focus
- Slower recall
- Greater mental fatigue
At the same time, repeated sugar exposure activates the brain’s dopamine system — a mechanism amplified by hyperpalatable foods that hijack reward pathways beyond normal satiety signals. Sugar stimulates reward pathways designed to reinforce survival behaviors. When activation is frequent, dopamine receptors can become less sensitive. The brain compensates by seeking stronger or more frequent stimulation.
This is not addiction in a dramatic sense. It’s adaptation.
Motivation shifts. Satisfaction thresholds rise. Smaller rewards feel less rewarding.
Then there is neuroinflammation.
Chronic blood sugar elevation increases inflammatory signaling throughout the body, including in the brain, where neuroinflammation can alter cognitive clarity and stress sensitivity. Even low-grade inflammation can affect mood regulation, stress sensitivity, and cognitive resilience.
The brain becomes more reactive to stress, resembling patterns in prolonged fight-or-flight mode where recovery signals are suppressed.. Energy fluctuations feel more intense. Mood stability narrows.
At this point, sugar is no longer just influencing metabolism.
It is shaping perception.
And while these changes may not be visible, the skin often reflects similar underlying processes — where structural proteins begin to respond to the same biochemical environment.
Fourth Shift: Structural Aging Through Glycation

While the brain adapts to instability, the skin reflects something different: structural change.
One of the most direct biochemical effects of excess circulating glucose is glycation.
Glycation occurs when glucose molecules bind to proteins in the body without enzymatic control. In the skin, those proteins are primarily collagen and elastin — the fibers responsible for firmness and elasticity.
When glucose binds to them, it forms compounds known as advanced glycation end products (AGEs).
These compounds stiffen collagen fibers. They reduce elasticity. They make the skin less resilient to mechanical stress and slower to repair.
Over time, this contributes to:
- Fine lines that deepen more quickly
- Reduced skin bounce and firmness
- Increased dullness
- Slower wound healing
Unlike dehydration or temporary irritation, glycation alters structure.
There is also an inflammatory component. Elevated blood sugar increases oxidative stress, which further damages collagen and impairs the skin barrier. In individuals prone to acne, insulin elevation can stimulate androgen production, increasing oil output and inflammatory breakouts.
These shifts don’t require extreme sugar intake. They are driven by repeated glucose elevation over time.
The skin becomes a visible surface of deeper metabolic signaling.
And once sugar begins acting not just as fuel, but as a daily stabilizer for mood and energy, the pattern reinforces itself — which is where behavior and physiology merge.
When Sugar Becomes a Daily Regulator

At this stage, the issue is no longer just biochemical. It becomes behavioral.
When blood sugar is unstable, the liver is overloaded, and dopamine signaling is dulled, sugar starts serving a different function.
It becomes a regulator.
Not consciously — physiologically.
You reach for it when energy dips.
When stress rises.
When focus fades.
When mood drops.
And it works — temporarily.
Glucose rises. Dopamine lifts. Cortisol stabilizes. You feel clearer, calmer, more functional.
But because the underlying signaling remains unstable, the relief doesn’t last. The crash follows. And the cycle repeats.
This is how excess becomes normalized.
Sugar shifts from being an occasional pleasure to being:
- A stress buffer
- A fatigue patch
- A mood corrector
- A reward substitute
Over time, the body begins anticipating those corrections. Hunger cues blur. Cravings intensify not because of weakness, but because regulatory systems are trying to maintain equilibrium.
The system is not addicted in a dramatic sense.
It is compensating.
And as long as compensation is required multiple times per day, the signaling environment that created the instability remains in place.
Which raises the practical question:
How much is too much — and how do you know when you’ve crossed that threshold?
What “Excess” Actually Means

“Excess” is not a moral judgment. It’s a physiological threshold.
For most people, excess sugar is not a single dessert. It’s a pattern of repeated glucose elevation without enough time for the system to reset.
Health guidelines generally suggest limiting added sugars to below 10% of daily calories, with additional metabolic benefits seen below 5%. In practical terms, that limit can be exceeded quickly through sweetened drinks, flavored yogurts, sauces, snack bars, cereals, and baked goods — even when the overall diet appears reasonable.
But numbers alone don’t tell the full story.
Excess usually looks like:
- Multiple blood sugar spikes per day
- Liquid sugar that bypasses satiety signals
- Carbohydrates consumed without protein or fat
- Late-night intake that disrupts circadian rhythm
- Using sugar to correct energy or mood dips
It is the frequency that matters most.
When insulin has time to return to baseline between meals, metabolic flexibility is preserved. When glucose exposure is constant, regulation becomes strained.
It is also important to distinguish added sugars from sugars found in whole foods.
Fruit contains fiber, water, and polyphenols that slow absorption and reduce glycemic load. The metabolic impact of an apple is not equivalent to that of a sugar-sweetened beverage.
Excess, then, is not defined by fear of sweetness.
It is defined by repeated signaling without recovery.
And when that pattern has been in place for years, the goal is not restriction — it is recalibration.
Which brings us to the final step: how to restore stability without triggering rebound cravings or metabolic stress.
Rebuilding Metabolic Resilience

Restoring stability is not about cutting sugar overnight. It’s about restoring the conditions that allow your body to regulate on its own.
The first priority is blood sugar consistency.
Eating balanced meals — with adequate protein, healthy fats, and fiber — slows glucose absorption and reduces sharp insulin spikes. When energy rises gradually instead of rapidly, crashes become less frequent. As crashes decline, the stress response quiets.
Next is reducing liquid sugar.
Sugar-sweetened beverages create the fastest glucose elevations because they lack fiber and require minimal digestion. Replacing soda, juice, and sweetened coffee drinks is often the most impactful first change.
Then comes meal spacing.
Allowing time between meals gives insulin levels space to return to baseline, supporting metabolic flexibility and cellular repair mechanisms that become more active during structured fasting periods.. This helps restore metabolic flexibility — the ability to shift between burning glucose and stored fat without triggering stress hormones.
Sleep also plays a central role.
Poor sleep increases hunger hormones and reduces satiety signaling. In that state, cravings for quick carbohydrates intensify. Improving sleep quality often reduces sugar intake naturally, without strict restriction.
Finally, focus on nutrient density rather than deprivation.
Minerals such as magnesium, potassium, and sodium support nerve function and stress recovery. Whole foods rich in protein and micronutrients provide the raw materials for stable energy regulation.
The goal is not perfection.
It is restoring responsiveness.
When insulin signaling improves, dopamine sensitivity recalibrates, and inflammation decreases, smaller amounts of sugar produce satisfaction again. The system becomes less reactive, more resilient.
And resilience — not restriction — is what prevents excess from becoming chronic.
The Quiet Accumulation Effect

None of these shifts happen overnight.
There is no single meal that causes insulin resistance. No single soda that alters dopamine signaling. No single dessert that stiffens collagen.
The change is cumulative.
Repeated blood sugar spikes strain regulation. Repeated liver overload increases fat storage. Repeated inflammatory signaling lowers resilience. Each shift is subtle. Together, they alter baseline function.
This is why dysfunction often develops long before diagnosis.
Fasting glucose may still fall within a “normal” range. Body weight may not raise concern. Yet fasting insulin may be elevated. Triglycerides may be trending upward. Energy stability may already be compromised.
The body adapts quietly — until it can’t compensate as effectively.
The purpose of understanding this is not alarm.
It is awareness of pattern.
Metabolic systems are dynamic. They respond to inputs over time. When added sugar intake decreases and nutrient density increases, insulin sensitivity can improve. Liver fat can decline. Inflammatory signaling can settle. Cognitive clarity can return.
The body is not fragile. It is responsive.
But responsiveness depends on cumulative exposure.
Sugar is not inherently harmful. Chronic excess is.
And when signaling stabilizes, the systems that were once reactive — metabolism, brain, skin — begin to regain flexibility.
Not through restriction.
Through regulation.
Final Thoughts

If there’s one misconception to leave behind, it’s the idea that this is about demonizing sugar.
It isn’t.
Sugar is a simple carbohydrate. The body knows how to process it. The problem arises when modern availability, food engineering, and daily stress combine to make high intake normal — and recovery rare.
What matters most is not a single number, a single food, or a single rule.
It’s whether your metabolic system feels stable.
Stable energy.
Stable mood.
Stable hunger cues.
Stable sleep.
When those are in place, occasional sugar is handled without disruption. When they’re not, even moderate intake can amplify instability.
The goal, then, isn’t rigid avoidance.
It’s restoring enough flexibility that your body doesn’t rely on sugar to regulate itself.
That shift — from reactivity to resilience — changes everything.
Because when signaling is steady, the brain is clearer.
The skin repairs more efficiently.
Hormones fluctuate less dramatically.
Energy becomes predictable again.
And at that point, sugar returns to what it was always meant to be:
An input.
Not a regulator.